Die Gürtelrose, auch als Herpes Zoster bekannt, kann nicht nur die Haut betreffen, sondern sie kann sich auch in der Mundregion manifestieren. Dies führt oft zu unangenehmen Symptomen und beeinträchtigt das tägliche Leben. Gürtelrose im Mund ist eine weniger bekannte Form dieser Krankheit, die jedoch ernsthafte Beschwerden verursachen kann. Um dir bei den verschiedenen Aspekten dieser Erkrankung zu helfen, bietet dieser Artikel wichtige Informationen zu Symptomen, Behandlungsmethoden und Vorbeugemöglichkeiten.
Symptome der Gürtelrose im Mund erkennen
Die Symptome der Gürtelrose im Mund können sehr unangenehm sein und variieren in ihrer Intensität. In der Regel treten zuerst allgemeine Symptome wie Fieber, Kopfschmerzen und ein allgemeines Unwohlsein auf. Diese ersten Anzeichen werden oft von einem brennenden oder stechenden Gefühl im Mund begleitet, welches auf die Nervenentzündung zurückzuführen ist. Ein charakteristisches Merkmal sind auch bläschenartige Ausschläge, die innerhalb weniger Tage erscheinen können.
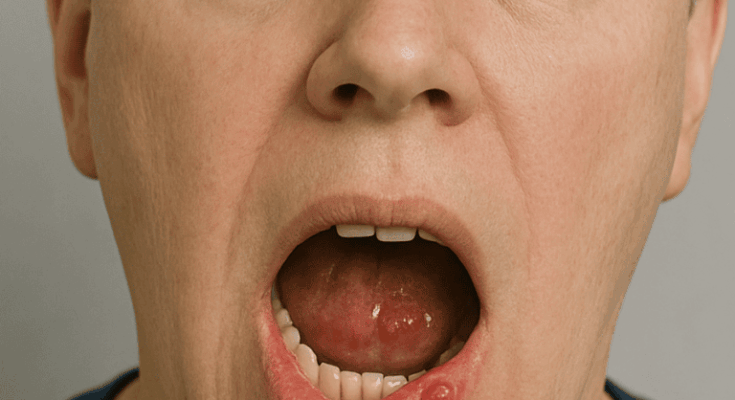
Diese Bläschen lassen sich häufig an den inneren Wangen, Lippen oder am Gaumen finden und verursachen massive Schmerzen. Das Essen, Trinken und Sprechen kann aufgrund dieser Symptome stark beeinträchtigt werden. Zusätzlich kann es zu Schwellungen im betroffenen Bereich kommen. Eine ernsthafte Komplikation ist die Möglichkeit, dass sich die Infektion auf andere Körperteile ausbreitet. Um eine bessere Vorstellung von diesem Zustand zu bekommen, können Gürtelrose im Mund Bilder hilfreich sein, da sie visuell darstellen, wie diese Erkrankung aussehen kann.
Ausführlicher Artikel: Fitness Verband » Stärke deine Karriere im Fitnessbereich
Gürtelrose im Mund Bilder zur Veranschaulichung
Um ein besseres Verständnis für die Gürtelrose im Mund zu erlangen, können Bilder sehr aufschlussreich sein. Sie veranschaulichen das typische Erscheinungsbild der Bläschen und Rötungen, die bei dieser Erkrankung auftreten. Oft sind sie an den inneren Wangen, den Lippen oder dem Gaumen sichtbar und zeigen eine erkennbare Schwellung. Das Anschauen solcher Bilder hilft dir, die Symptome leichter zu erkennen. Dabei ist es wichtig, sich bewusst zu machen, dass jeder Fall individuell unterschiedlich sein kann. Einige Menschen erleben schwerere Symptome, während andere milder betroffen sind. Es gibt auch Unterschiede in der Ausbreitung der Blasen, die bei verschiedenen Patienten variieren können.
Darüber hinaus können diese Abbildungen dazu beitragen, Ängste abzubauen, indem sie dir zeigen, was genau zu erwarten ist, falls du betroffen bist. Die visuelle Darstellung ermöglicht eine bessere Kommunikation mit Ärzten und medizinischem Personal, um die bestmögliche Behandlung zu gewährleisten. Daher sind diese Bilder nicht nur informativ, sondern auch nützlich für Betroffene und deren Angehörige.
| Symptome | Behandlung | Vorbeugung |
|---|---|---|
| Fieber und Kopfschmerzen | Antivirale Medikamente | Impfung gegen Gürtelrose |
| Brennende Schmerzen im Mund | Schmerzlindernde Mittel | Stressmanagement |
| Bläschenbildung | Topische Behandlungen | Gesunde Ernährung |
Behandlungsmethoden der Erkrankung
Die Behandlung von Gürtelrose im Mund erfordert oft eine Kombination verschiedener Ansätze. Eine der gängigsten Methoden sind antivirale Medikamente, die frühzeitig eingenommen werden sollten, um das Virus zu bekämpfen und die Dauer der Symptome zu verkürzen. Diese Medikamente können helfen, den Verlauf der Erkrankung abzuschwächen und die Bildung neuer Bläschen zu verhindern. Zusätzlich können schmerzlindernde Mittel eingesetzt werden, um die Beschwerden zu lindern. Diese Schmerzmittel unterstützen dabei, das tägliche Leben erheblich zu vereinfachen. Dazu gehören sowohl rezeptfreie als auch verschreibungspflichtige Optionen, je nach Schweregrad der Schmerzen.
Zur Unterstützung der Heilung bietet sich auch die Verwendung von topischen Behandlungen an. Diese Lösungen oder Salben können direkt auf die betroffenen Stellen aufgetragen werden, um Entzündungen zu reduzieren und die Heilung zu fördern. Es ist wichtig, bei den ersten Anzeichen einer Gürtelrose im Mund einen Arzt aufzusuchen. Nur so kann eine angemessene Behandlung rechtzeitig begonnen werden, um mögliche Komplikationen zu vermeiden. In jedem Fall spielt eine frühe medizinische Intervention eine entscheidende Rolle bei der Linderung der Symptome und der Förderung einer schnellen Genesung.
Schmerzmanagement für betroffene Personen
Das Schmerzmanagement für Personen mit Gürtelrose im Mund spielt eine entscheidende Rolle in der täglichen Bewältigung dieser Erkrankung. Die Schmerzen können auf verschiedene Weise beeinträchtigen, weshalb gezielte Maßnahmen notwendig sind. Eine häufig empfohlene Maßnahme sind rezeptfreie Schmerzmittel. Diese Medikamente können schnell zur Linderung beitragen und somit das Wohlbefinden steigern. Auch ärztlich verschriebene Schmerzmittel kommen zum Einsatz, wenn die Beschwerden schwerwiegender sind. Daher ist es wichtig, den Schweregrad der Symptome zu bewerten und gegebenenfalls Rücksprache mit einem Arzt zu halten.
Zusätzlich sollte ein sanftes Mundpflege-Regime beachtet werden, um Irritationen zu minimieren. Dazu gehört das Vermeiden von scharfen oder sehr heißen Speisen, da diese Reizungen hervorrufen können. Eine ausgewogene Ernährung, unterstützt durch weiche Lebensmittel, trägt ebenfalls zur Minderung des Schmerzes bei. Entspannungsübungen könnten ebenso hilfreich sein, um allgemeine Stresssymptome abzubauen. Durch diese Techniken lässt sich das körperliche Empfinden verbessern und möglicherweise auch die Wahrnehmung der Schmerzen verringern. Es ist ratsam, stets aufmerksam auf die eigenen Bedürfnisse zu hören und rechtzeitig Maßnahmen zur Linderung zu ergreifen.
Die Gesundheit ist der größte Reichtum. Achte darauf, was du deinem Körper und Geist zufügst. – Buddha
Zusätzlicher Lesestoff: Depression verstehen und überwinden: Wie Online-Therapie dir helfen kann
Vorbeugende Maßnahmen zur Reduzierung des Risikos
Um das Risiko einer Gürtelrose im Mund zu reduzieren, kannst du verschiedene vorbeugende Maßnahmen ergreifen. Eine wichtige Maßnahme ist die Impfung gegen Gürtelrose. Diese Impfung kann dir helfen, eine Infektion mit dem Virus zu verhindern oder den Verlauf der Erkrankung erheblich zu mildern, falls es dennoch zu einer Infektion kommt. Zusätzlich spielt ein starkes Immunsystem eine entscheidende Rolle. Achte darauf, dich gesund zu ernähren und ausreichend Bewegung in deinen Alltag zu integrieren. Dazu gehört auch genügend Schlaf, um deinem Körper die benötigte Regeneration zu ermöglichen.
Stressmanagement ist ebenfalls bedeutend, denn erhöhter Stress kann das Risiko für viele Erkrankungen erhöhen. Techniken wie Meditation oder Yoga können hier wertvolle Unterstützung bieten. Ein weiterer wichtiger Punkt ist der regelmäßige Kontakt zu einem Arzt. Durch regelmäßige Vorsorgeuntersuchungen lassen sich potenzielle gesundheitliche Probleme frühzeitig erkennen und behandeln. Besonders Personen, die bereits einmal an Gürtelrose erkrankt sind, sollten deren Symptomatik ernst nehmen und auf ihren Gesundheitszustand achten, um mögliche Rückfälle zu vermeiden.
Zum Weiterlesen: Aufklärungspflicht von Ärzten – Was muss vor einer Behandlung kommuniziert werden?
Informationen zu weiteren medizinischen Unterstützungsmöglichkeiten
Wenn du unter Gürtelrose im Mund leidest, kann eine umfassende medizinische Unterstützung entscheidend zur Linderung deiner Symptome beitragen. Neben der klassischen Behandlung durch einen Arzt gibt es zusätzliche Ressourcen, die dir helfen können. Ärztliche Beratung ist unerlässlich. Der Besuch bei einem spezialisierten Arzt oder Zahnarzt kann wertvolle Einblicke und individuelle Behandlungspläne bieten. Diese Fachleute können auf deine spezifischen Symptome eingehen und gegebenenfalls alternative Therapien vorschlagen. Ein weiterer Ansatz könnte die Konsultation eines Ernährungsberaters sein.
Eine ausgewogene Ernährung kann zur Verbesserung des Immunsystems beitragen und die Heilung unterstützen. Es gibt spezielle Lebensmittel, die entzündungshemmende Eigenschaften haben und somit zur Schmerzlinderung führen können. Auch physiotherapeutische Verfahren können in bestimmten Fällen hilfreich sein. Physio- oder Ergotherapeuten können Übungen anleiten, die dazu beitragen, Verspannungen zu lösen und das allgemeine Wohlbefinden zu steigern. Die gute Zusammenarbeit mit unterschiedlichen Gesundheitsdienstleistern kann den Heilungsprozess unterstützen und die Lebensqualität verbessern.